Table of contents
- KEY TAKEAWAYS
- A Failed IVF Cycle Does Not Mean the End — Here Is Why
- QUICK FACTS
- PCMC IVF Failure Statistics 2025-2026
- Reason 1 — Poor Egg Quality
- Reason 2 — Poor Embryo Development in the Lab
- Reason 3 — Implantation Failure
- Reason 4 — Uterine Abnormalities
- Reason 5 — Sperm DNA Fragmentation
- Reason 6 — Incorrect Stimulation Protocol
- Reason 7 — Thrombophilia or Immunological Factors
- IVF Failure Investigation Protocol at Dr. Shitole’s PCMC Clinic
- IVF Failure and Next Steps in PCMC — Local Context
- Frequently Asked Questions
- Conclusion
KEY TAKEAWAYS
Poor egg quality is the most common cause of IVF failure — particularly in women over 35 or with low AMH.
Implantation failure — embryo does not attach to the uterine lining — accounts for a significant share of failed transfers even with good-quality embryos.
The ERA (Endometrial Receptivity Array) test identifies the exact window of implantation for personalised embryo transfer timing.
Sperm DNA fragmentation — often undetected on standard semen analysis — can cause fertilisation failure or early embryo arrest.
Uterine abnormalities such as polyps, fibroids or a thin endometrium must be corrected before attempting a further IVF cycle.
After 2 to 3 failed IVF cycles in PCMC, a comprehensive failed cycle review with Dr. Shitole is essential before proceeding.
A Failed IVF Cycle Does Not Mean the End — Here Is Why
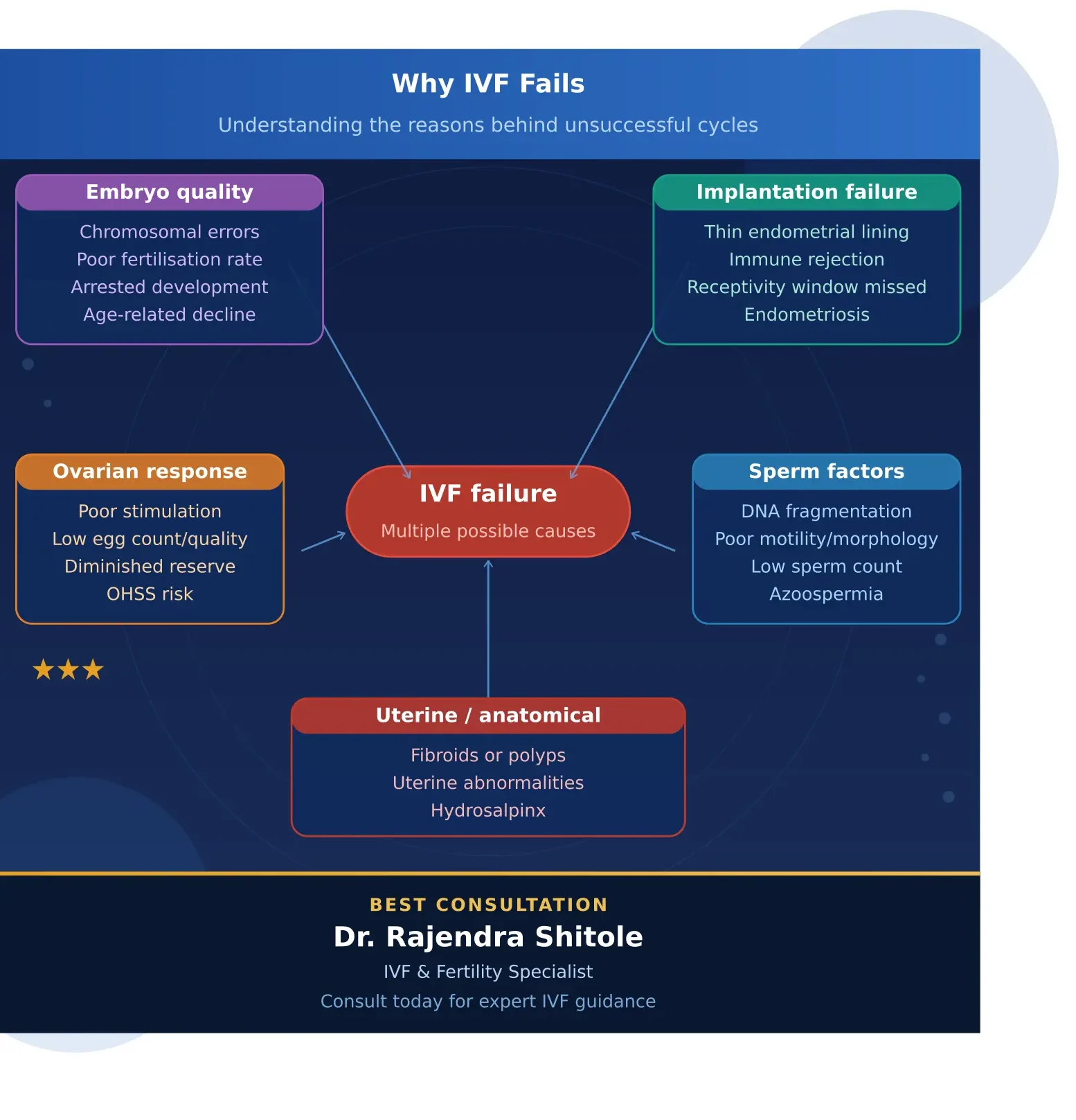
Why IVF fails in PCMC is the most painful question Dr. Shitole’s team receives. After weeks of injections, monitoring, hope and the transfer itself — a negative pregnancy test is devastating. But a failed IVF cycle is also clinical data. Every failure narrows the diagnostic picture and points toward a specific cause that can be addressed in the next attempt.
The overall IVF failure rate per cycle is approximately 35 to 45 percent even at the best clinics (ICMR 2024). Most couples who succeed with IVF do so after 1 to 3 attempts. Understanding why your cycle failed is the most important step you can take before trying again. This guide, reviewed by Dr. Rajendra Shitole — IVF specialist in PCMC — explains the 7 most common reasons IVF fails and what advanced rescue protocols are available at his Pimpri-Chinchwad clinic.
QUICK FACTS
IVF failure rate per cycle (any age): 35 to 45 percent (ICMR 2024)
Most common cause of failure: Poor egg or embryo quality
Implantation failure share of overall failures: Approx. 30 to 40 percent
ERA test cost in PCMC: INR 25,000 to 40,000
Sperm DNA fragmentation test cost: INR 3,000 to 6,000
Success rate after failed cycle review and protocol adjustment: Significantly improved
PCMC IVF Failure Statistics 2025-2026
| Metric | Data Point | Source |
| IVF failure rate per cycle | 35 to 45 percent | ICMR 2024 |
| Implantation failure share of all failures | Approx. 30 to 40 percent | Industry estimate |
| Egg quality as primary failure cause | Most common single factor | Industry estimate |
| Sperm DNA fragmentation in failed IVF couples | Up to 25 percent | PubMed 2021 |
| Uterine abnormality found on failed cycle review | 20 to 25 percent of cases | Industry estimate |
| ERA test accuracy for implantation window | Approx. 90 percent | PubMed 2022 |
| Success rate improvement after failed cycle review | Significant in protocol-adjusted cycles | Industry estimate |
Reason 1 — Poor Egg Quality
Egg quality is the single most common reason for IVF failure. As women age — particularly after 35 — a higher proportion of eggs carry chromosomal abnormalities. These eggs either fail to fertilise, arrest during embryo development, or produce embryos that fail to implant or result in early miscarriage.
Solution at Dr. Shitole’s PCMC clinic: PGT-A (Preimplantation Genetic Testing for Aneuploidies) screens embryos for chromosomal errors before transfer — only chromosomally normal embryos are transferred, dramatically improving per-transfer success rates. For women over 40 or with repeated failure, donor egg IVF eliminates the egg quality problem entirely.
Reason 2 — Poor Embryo Development in the Lab
Even with good eggs and sperm, not all embryos develop well to blastocyst stage. Some arrest at Day 3 — never reaching the transfer-ready Day 5 blastocyst. Poor embryo development can reflect egg quality, sperm quality, fertilisation technique or laboratory conditions.
Solution: Dr. Shitole’s clinic uses time-lapse incubation — embryos develop in an uninterrupted environment and are monitored with continuous imaging without disturbance. The time-lapse algorithm identifies the embryos most likely to implant successfully. ICSI is used for fertilisation in all cases where sperm quality is a concern.
Reason 3 — Implantation Failure
A good-quality embryo can still fail to implant if the uterine lining is not receptive at the exact time of transfer. The endometrium has a narrow window of receptivity — called the Window of Implantation (WOI) — that lasts only 24 to 48 hours per cycle. In approximately 1 in 4 women, this window is displaced from the standard Day 5 post-ovulation timing.
Solution: The ERA (Endometrial Receptivity Array) test analyses a small endometrial biopsy using gene expression profiling to identify the exact WOI for an individual woman. Transfers are then scheduled to match the personalised window. ERA-guided transfers have been shown to significantly improve implantation rates in women with recurrent implantation failure (PubMed 2022).
Reason 4 — Uterine Abnormalities
Polyps, submucosal fibroids, uterine septa, adhesions (Asherman’s syndrome) and a thin endometrium all reduce implantation rates. These may be present but missed on standard ultrasound — particularly small polyps or mild adhesions.
Solution: Before any further IVF cycle after failure, Dr. Shitole recommends a hysteroscopy to directly inspect the uterine cavity. Any correctable abnormality is treated in the same sitting. A saline infusion sonography (SIS) scan is offered as a less invasive screening step before hysteroscopy.
Reason 5 — Sperm DNA Fragmentation
Standard semen analysis measures sperm count, motility and morphology — but not DNA integrity. Sperm with high DNA fragmentation (above 25 to 30 percent DFI) can fertilise an egg but produce embryos with arrested development or abnormal chromosomes. This is a hidden cause of IVF failure that is missed unless specifically tested.
Solution: Sperm DNA fragmentation testing (DFI test) costs INR 3,000 to 6,000 at Dr. Shitole’s PCMC clinic. If DFI is high, a course of antioxidant supplements (CoQ10, Vitamin E, Vitamin C, Lycopene) for 3 months can improve DNA integrity. Surgical sperm retrieval (TESA) may also be recommended in selected cases, as testicular sperm has lower DNA fragmentation than ejaculated sperm.
Reason 6 — Incorrect Stimulation Protocol
An IVF protocol that produces too few eggs, too many eggs, or eggs with poor maturation quality can result in poor embryo outcomes despite healthy underlying fertility. Poor response to stimulation (fewer than 3 eggs retrieved) or hyper-response with OHSS both compromise cycle outcomes.
Solution: Every failed cycle at Dr. Shitole’s clinic is reviewed with the embryology team. Stimulation dose, trigger timing, embryo development data and transfer timing are all examined. Protocol adjustments — including dose changes, trigger type, luteal phase support modifications and dual stimulation for poor responders — are planned for the next cycle.
Reason 7 — Thrombophilia or Immunological Factors
In a small proportion of women with recurrent IVF failure, underlying blood clotting disorders (thrombophilia) or immunological abnormalities prevent embryo implantation. Conditions like antiphospholipid syndrome (APS), Factor V Leiden mutation and elevated NK cells have been associated with recurrent implantation failure.
Solution: After 2 to 3 failed cycles, Dr. Shitole recommends a thrombophilia screen and antiphospholipid antibody panel. If abnormalities are found, low-molecular-weight heparin, low-dose aspirin or immunotherapy protocols are added to the next IVF cycle to support implantation.
IVF Failure Investigation Protocol at Dr. Shitole’s PCMC Clinic
| Investigation | What It Detects | When Recommended |
| ERA test | Displaced window of implantation | After 2 or more failed transfers with good embryos |
| Hysteroscopy | Uterine cavity abnormalities | After any failed cycle — especially with good embryos |
| Sperm DNA fragmentation test | High DNA damage in sperm | After failed cycle with poor embryo development |
| PGT-A testing | Chromosomal abnormalities in embryos | After age-related or recurrent failure |
| Thrombophilia and APS screen | Blood clotting and immune disorders | After 2 to 3 failed cycles |
| Thyroid and prolactin recheck | Hormonal causes of implantation failure | After any failed cycle |
| Endometrial scratch | Triggers implantation-promoting response | In selected recurrent failure cases |
IVF Failure and Next Steps in PCMC — Local Context
Couples in PCMC who have experienced IVF failure often feel pressure to try again immediately — or conversely, to give up entirely. Dr. Shitole’s clinic provides a structured failed cycle review consultation after every unsuccessful transfer. This review takes 30 to 45 minutes, covers all cycle data and produces a clear written plan for the next attempt.
A couple from Hinjewadi — both IT professionals — came to Dr. Shitole after two failed IVF cycles at another clinic. A hysteroscopy revealed a small uterine polyp missed on earlier scans. After removal and an ERA-guided transfer, their next IVF cycle was successful. The investigation cost them INR 45,000 and saved them from a third unsuccessful cycle.
Frequently Asked Questions
- Q: How many IVF failures before giving up in PCMC?
There is no universal number. After each failed cycle, a review identifies modifiable factors. Most couples who go through a systematic failed cycle investigation find a correctable cause — and succeed in a subsequent attempt. Dr. Shitole guides every couple through this process with honesty about realistic expectations.
- Q: What tests should I do after a failed IVF in PCMC?
A: After a failed IVF cycle, the key investigations are: hysteroscopy to check the uterine cavity, sperm DNA fragmentation test, ERA test if two or more embryo transfers have failed, PGT-A if egg quality is suspected, and thrombophilia and APS screen if recurrent failure is present. Dr. Shitole will prioritise these based on your specific cycle history.
- Q: Can IVF fail even with good embryos?
A: Yes. Good embryo quality is necessary but not sufficient for implantation. The uterine environment must also be receptive at exactly the right time. ERA testing, hysteroscopy and thrombophilia screening address the uterine and systemic factors that prevent implantation despite good embryos.
- Q: What is the ERA test and does it improve IVF success after failure?
A: The ERA (Endometrial Receptivity Array) test takes a small biopsy of the uterine lining in a mock cycle to identify the exact window of implantation for that individual woman. For women whose WOI is displaced from the standard timing, ERA-guided transfer significantly improves implantation rates (PubMed 2022). It costs INR 25,000 to 40,000 in PCMC.
- Q: Is sperm DNA fragmentation tested in standard semen analysis?
A: No. Standard semen analysis measures count, motility and morphology — not DNA integrity. Sperm DNA fragmentation (DFI) is a separate test costing INR 3,000 to 6,000. It’s recommended after failed IVF cycles where embryo development was poor despite adequate fertilisation.
- Q: Should I try IVF again after two failures in PCMC?
A: After two failed cycles, a systematic failed cycle review is strongly recommended before a third attempt. Proceeding without investigation risks repeating the same outcome. With investigation and protocol adjustment, success rates for the third cycle are often significantly better than the first two.
Conclusion
Why IVF fails in PCMC is a question with real, investigable and often correctable answers. Poor egg quality, implantation failure, uterine abnormalities, sperm DNA damage, wrong protocol, thrombophilia and poor embryo development are all identifiable through targeted testing.
Dr. Rajendra Shitole at D.Y. Patil Hospital, Pimpri-Chinchwad offers a comprehensive failed IVF cycle review and rescue protocol service. If your IVF cycle has failed, the next step is not despair — it’s a 30-minute consultation that may change everything.
Dr. Rajendra Shitole
Dr. Rajendra Shitole, Best IVF & Fertility Specialist Centre in PCMC . is a highly skilled Gynaecologist, Fertility Consultant, and Laparoscopic & Robotic Surgeon with over 11 years of experience dedicated to women’s health and reproductive care. His mission is to help childless couples fulfill their dream of parenthood through compassionate care and advanced medical expertise.
He has successfully managed numerous complex cases of Infertility, Fibroids, PCOS, Adenomyosis, Endometriosis, and Male Factor Infertility.
